Oxycodone Addiction, Effects, Withdrawal, & Rehab
Oxycodone is a prescription opioid used to treat moderate to severe pain. It’s the main ingredient in brand-name drugs such as OxyContin and Percocet.1,2
Like other prescription opioids, oxycodone can be a safe and effective means of pain management when used properly and for a short period of time. However, it may have some significantly negative health effects, and can be extremely dangerous when abused.2
How Does Oxycodone Misuse Start?
In addition to altering pain signaling, oxycodone and other opioids are associated with an increase in dopamine activity in the brain.2
When opioids are used in high enough doses, the accompanying increase in dopamine helps elicit a rewarding, euphoric high. This in turn may reinforce continued use—and misuse—of oxycodone and other drugs like it, even in some who originally began taking the drug for medical purposes.2
Others may never have been prescribed oxycodone and purely started misusing prescription painkillers to get high.
Misuse of oxycodone means any of the following:3,4
- Taking someone else’s prescription or otherwise acquiring the drug illegally.
- Taking oxycodone or another medication containing oxycodone for non-medical reasons, such as to get high.
- Using oxycodone more frequently, for longer, or in higher doses than prescribed.
- Using oxycodone in an unintended way (e.g., crushing pills and snorting or injecting them).
What Is Oxycodone?
Oxycodone is a semi-synthetic opioid widely used as a prescription painkiller. Oxycodone and other opioids bind to opioid receptors to modify pain messages sent between the brain and the body.2
Brand name formulations that contain oxycodone include:
- OxyContin.
- Percocet.
- Roxicodone.
- Xtampza ER.
The U.S. Drug Enforcement Administration (DEA) considers oxycodone a Schedule II controlled substance, meaning it has valid medical uses but also high abuse potential.5
Effects of Oxycodone
Oxycodone use and misuse can affect a person’s health and well-being. The most common oxycodone side effects include:1
- Nausea.
- Constipation.
- Vomiting.
- Headache.
- Itchiness.
- Insomnia.
- Dizziness.
- Weakness or lethargy.
- Drowsiness.
Oxycodone Overdose
Overdose is a serious risk of oxycodone misuse. The signs and symptoms of a possible oxycodone overdose include:1,6,7
- Slowed or stopped breathing.
- Extreme drowsiness or lack of consciousness.
- Limp body.
- Cold, clammy, or bluish skin.
- Vomiting.
- Choking or gurgling sounds.
- Pinpoint pupils.
Mixing prescription opioids like oxycodone with benzodiazepines, alcohol, or other central nervous system (CNS) depressants is dangerous and can increase the risk of overdose and death.
Narcan (naloxone) is a life-saving nasal spray drug that can reverse the effects of an opioid overdose. If you have access to Narcan in the event of an opioid overdose, administer it right away and wait until help arrives.
Oxycodone Detox & Withdrawal Symptom Management
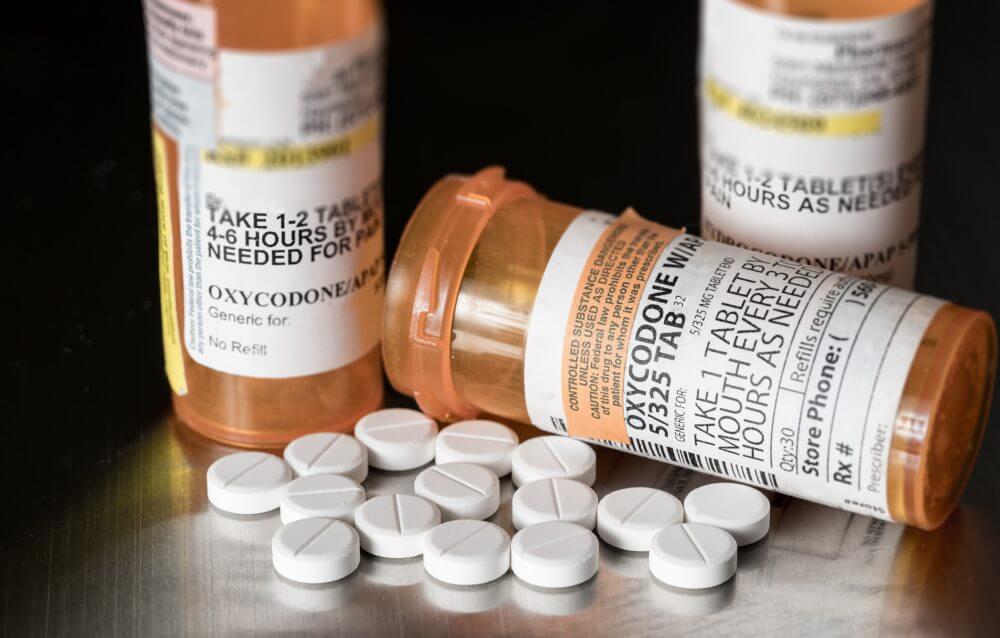
Many who struggle with oxycodone addiction develop significant physiological dependence, which places them at risk of withdrawal if opioid use is suddenly stopped or reduced. Opioid withdrawal can be severe and uncomfortable.1,2
The supportive care and pharmaceutical interventions offered through a supervised medical detox program can help people through this difficult period of early recovery.
Oxycodone Withdrawal Symptoms
Common oxycodone withdrawal symptoms may include:1,8,9
- Restlessness.
- Yawning.
- Runny nose.
- Teary eyes.
- Sweating.
- Chills.
- Muscle aches and pain.
Other signs and symptoms may include:1,8,9
- Irritability.
Anxiety. - Backache.
- Joint pain.
- Weakness.
- Abdominal cramps.
- Insomnia.
- Nausea and vomiting.
- Diarrhea.
- Elevated vitals (e.g., blood pressure, respiratory rate, and heart rate).
The character and severity of these symptoms may vary according to the degree of physical dependence, but may also be influenced by a person’s general health.10
For relatively short-acting opioids like oxycodone, withdrawal symptoms typically start between 8–24 hours after the last use and usually resolve within 4–10 days.10
Oxycodone withdrawal is rarely life-threatening. However, it can be very uncomfortable, which could increase relapse risks in people whose withdrawal symptoms are not mitigated. Medically assisted detox can make this process easier, as medical staff monitor patients and administer medication when necessary.9
While getting past the acute withdrawal stage is a necessary hurdle to overcome, there’s much more to addiction recovery than detoxification. After detox, many patients transition into a comprehensive inpatient or outpatient program.9,11
Oxycodone Addiction Treatment Near Oxford, MS
If you or a loved one is struggling with drug or alcohol addiction, professional treatment can help. At Oxford Treatment Center, our Mississippi inpatient drug & alcohol rehab provides personalized, evidence-based care designed to address the individual needs of each patient.
Contact us at to learn more about your treatment options, the different levels of addiction treatment we offer (including inpatient addiction treatment), rehab admissions, and more.
Our trained and compassionate admissions navigators can also help answer questions about drug and alcohol rehab insurance coverage or other rehab payment options.
You don’t have to live with addiction any longer. Make the call today.
American Addiction Centers (AAC) is committed to delivering original, truthful, accurate, unbiased, and medically current information. We strive to create content that is clear, concise, and easy to understand.
While we are unable to respond to your feedback directly, we'll use this information to improve our online help.