Prescription Drug Abuse
Prescription medications are prescribed by licensed medical practitioners, issued from a pharmacy, and intended for use only by one person. Prescription drugs are regulated by the U.S. Food & Drug Administration, which monitors substances closely due to potential dangers and prescription drug abuse.1
Prescription medicines are a significant part of our nation’s healthcare expenditures. The Department of Health and Human Services estimated U.S. prescription drug spending in 2018 to reach $535 billion.2 Americans are also avid users of prescription drugs. As of the 2011 United Nations World Drug Report, Americans make up 5% of the world’s population yet use 75% of the world’s prescription medications3—and the vast majority of this use is legal.
Most prescription drugs are used correctly and not abused, and are a vital and important part of the United States healthcare system. However, prescription drugs can and are abused—to such a large extent in the U.S. that it’s been termed an epidemic.4
Certain prescription drugs carry a greater risk of abuse than others. These drugs, belonging chiefly to three medical classes, pose dangers for those who abuse them. Read on to learn more about the significant problems surrounding the abuse of prescription drugs.
How Common is Prescription Drug Abuse?
 After marijuana use, prescription drug misuse was the second most common form of illicit drug use in the U.S. in 2018.5
After marijuana use, prescription drug misuse was the second most common form of illicit drug use in the U.S. in 2018.5
Also stated in the SAMHSA report was the misuse of opioids, ringing in at 9.9 million users who misused prescription opioids in the U.S.5 In 2017, 67.8% of all drug overdose deaths—out of a total of 70,237—were caused by opioids.6
The number of overdose deaths involving opioids (including prescription opioids and illegal opioids like heroin and illicitly manufactured fentanyl) in 2017 was 6 times higher than in 1999. On average, 130 Americans die every day from an opioid overdose.4
In 2013, drug overdose became the leading cause of injury death in the U.S.7
If you’re worried that you or a loved one is abusing prescription drugs, there are ways to get help. Oxford Treatment Center and all of American Addiction Centers facilities utilize evidence-based treatment and therapies to help our patients reach recovery. Call our Admissions Navigators at for more information.
What Are Commonly Abused Prescription Drugs?
Many prescription drugs that are targeted for recreational use or abuse are notable for the strong effects the drugs can have on a user’s mind and body. Most belong to three categories.8
What Are the Signs of Prescription Drug Abuse?
There are several warning signs that medical professionals use to diagnose a substance use disorder. Below are the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition’s diagnostic criteria for a substance use disorder:9
- Substance is taken in increasing doses over longer period of time than was initially intended.
- There’s a persistent desire and maybe unsuccessful efforts to cut down and/or control use of the substance.
- User craves the substance.
- User spends a lot of time trying to get the substance.
- Substance use results in the user unable or choosing not to complete obligations or responsibilities.
- User continues substance use in spite of continuing social or relationship issues caused by use.
- User has given up on important activities and events because of use.
- Substance is used in situations where it is physically hazardous to do so.
- User continues substance use despite knowing of continual physical or psychological problems that are caused or worsened by use.
- User develops tolerance to substance.
- User has symptoms of withdrawal when not using.
Changes in how a person behaves or presents him or herself often occur with prescription drug abuse. These general changes can manifest as:
- Lying or misleading friends and loved ones about the use of prescription drugs
- Stealing or forging prescriptions to obtain more drugs
- Seeing a variety of doctors for additional prescriptions
- Changes in social circles
- Weight changes
- Deterioration in personal hygiene or appearance
- Financial issues
- Mood changes
While some individuals may not show many outward signs of abuse, most people exhibit some indications that should trigger further consideration among friends and loved ones.
Signs and symptoms of opioid abuse may include drowsiness, confusion, and slowed breathing rate. Signs and symptoms of benzodiazepine abuse may include slurred speech, poor concentration, and memory problems. Signs and symptoms of stimulant abuse include insomnia, anxiety, and paranoia.9
How Does Abuse Develop?
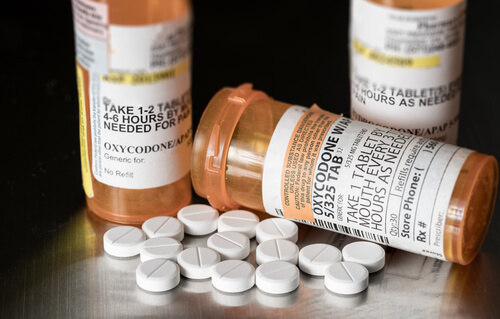 Often, legitimate prescription drug use can turn into abuse. In West Virginia, for example, a high percentage of people currently abusing prescription drugs started for legitimate medical purposes, often following a workplace accident. The state, like others in the Appalachia region, has a large number of blue-collar workers who often work in potentially dangerous fields, such as mining or construction, where injuries can be a common occurrence.
Often, legitimate prescription drug use can turn into abuse. In West Virginia, for example, a high percentage of people currently abusing prescription drugs started for legitimate medical purposes, often following a workplace accident. The state, like others in the Appalachia region, has a large number of blue-collar workers who often work in potentially dangerous fields, such as mining or construction, where injuries can be a common occurrence.
A person might get a prescription for Percocet or any oxycodone-based medication following an injury and initially take the medication as prescribed to relieve pain. Over time, a tolerance may develop, and the person may begin taking a larger dose to feel the drug’s effects. It’s important to remember that any deviation from the prescription’s instructions constitutes abuse.10
As people begin to use the drugs in higher-than-recommended doses, they may also be more likely to experiment with the routes with which they take the medication (such as crushing it to bypass extended-release formulations prior to snorting or injecting) or combine it with other substances to amplify the desired subjective effects.11
Some people simply begin using prescription drugs non-medically or recreationally. They may take pills left over from a legitimate prescription, or they may obtain pills from friends or family members. These individuals don’t have a valid need for the medication; they are simply taking it for the euphoria and calm that often accompany with use.
Abuse of prescription drugs—including opiates and benzodiazepines—can lead to addiction quickly. Since prescription painkillers are opiates, they are in the same class of drug as heroin and, similarly, have a very high addiction potential. Those who abuse prescription painkillers may be at higher risk of progressing to heroin use due to the similar desired effects of the drugs and the fact that heroin may be relatively cheaper and easier to obtain. Per NIDA, nearly 80% of U.S. heroin users reported prior prescription opioid use.12
Many who abuse prescription drugs mistakenly believe them to be safer than “street” drugs like heroin or cocaine because they are of pharmaceutical grade and initially prescribed by a doctor. While prescription drugs can be used safely as prescribed for legitimate medical purposes, some can be incredibly addictive.13
How Do People Stop Abusing Prescription Drugs?
While prescription drug abuse can lead to significant health, career, relationship, and financial repercussions,9 full recovery is possible. Addiction is a chronic disorder and, though there may be no easy “cure” for the disease, it can be managed with comprehensive and ongoing treatment.
Addiction is different for everyone, just as treatment for addiction should be.
Prescription Drug Detox
Medical detox is often the first step in the treatment process. Left unmanaged, withdrawal from certain substances, such as benzodiazepines and opiates, can be quite uncomfortable and even unsafe. In these instances, medical detox may be needed, as it might otherwise be risky to quit taking these substances suddenly on their own.9
Medical professionals will assess for the need for medical detox at the start of the rehabilitation period. If a person was taking prescription drugs to manage a physical or mental health disorder, doctors will use this information to inform the best treatment plan going forward. In some instances, clients may be switched to a different medication with less abuse potential. In other cases, alternative treatments, such as massage, physical therapy, or acupuncture, may be employed.14
Residential or Outpatient Treatment
After detox, many patients continue on with residential treatment where a treatment team can provide around-the-clock care as necessary. For those with strong support systems and who may have responsibilities they cannot shelf during treatment, outpatient treatment might be the right path.15
Either way, the bulk of addiction treatment takes place in the form of extensive counseling and therapy.16 In both individual and group therapy, clients explore the reasons behind their prescription drug abuse as well as strategies to end maladaptive and compulsive drug use behaviors. The specific program of care is catered to the individual, ensuring that treatment addresses the individual person’s progress in recovery.
It’s never too late to reach out for help. If you or someone you love is struggling with the devastating side effects of addiction and are unsure of where to turn, call us today at . Oxford Treatment Center, American Addiction Centers’ drug rehab in Mississippi, is ready to help you get the treatment you need today.
Aftercare
Aftercare is a key component to any successful recovery program. Prior to completion of a formal addiction treatment program, the treatment team will devise an aftercare plan for the client. The client and treatment team work on the plan together to ensure it meets the client’s needs on various levels, providing the support and structure needed for a successful long-term recovery.
American Addiction Centers (AAC) is committed to delivering original, truthful, accurate, unbiased, and medically current information. We strive to create content that is clear, concise, and easy to understand.
While we are unable to respond to your feedback directly, we'll use this information to improve our online help.